Hip dislocation
What is a dislocated hip?
The hip is comprised of a ball and socket joint. The ball (attached to the femur) sits in the acetabulum (socket) connected with the pelvis. The ball is kept in position by a combination of features including:
the acetabular dorsal rim (think of this like a roof)
the round ligament (think of this like a rope connecting the ball to the centre of the socket
joint capsule (think of this like glad wrap enveloping the ball and socket
What causes hip dislocation?
Dislocation of the hip occurs due to disruption of the normal connection between the ball and socket, this can occur due to:
trauma
conformation (poor design)
How is hip dislocation diagnosed?
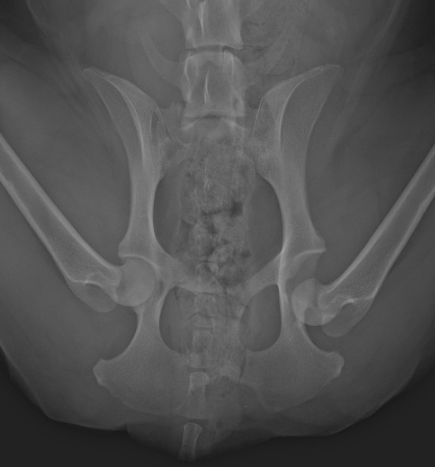
Hip dislocation is often suspected based on palpation of the normal bony structures of the hip joint and derangement of these structures. However the diagnosis is always confirmed on radiography (X-Rays).
The direction of the dislocation influences the choice of treatment and includes:
cranio-dorsal (forwards and upwards)
caudal-ventral (backwards and downwards)
A caudo-ventral hip dislocation
How do you treat hip dislocation?
The goal of managing hip dislocation is to restore the normal arrangement of the ball and socket, reduce the risk of osteoarthritis development and reduce the risk of subsequent dislocation events.
Options for management include:
Closed reduction (no surgery) where the hip is manipulated back into position
Open reduction (surgery) where torn tissue is cleaned from the joint, the hip is returned to its position and a synthetic ligament is inserted to maintain it in its new position
Femoral head ostectomy (FHO) where the ball is removed surgically
Total hip replacement (THR) where a new hip is inserted
The success rates of open vs closed reduction vary depending on the direction of dislocation. Caudal-ventral (backwards and downwards) have a more than 75% success rate with closed reduction. Whilst most cranio-dorsal (forwards and upwards) luxations are best treated with open reduction.
When surgery is necessary, and hip conformation is acceptable, then open reduction is often recommended. When surgery is necessary, and hip conformation is unacceptable, then total hip replacement is recommended. We rarely advocate for FHO due to the unpredictability of outcome and potential for ongoing lameness.
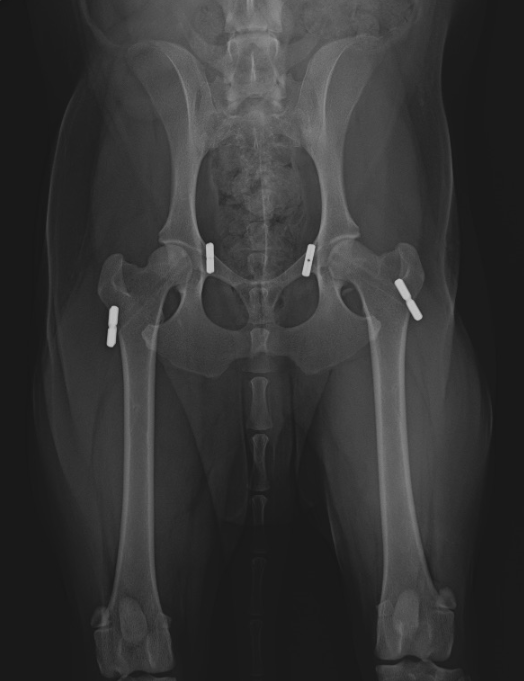
Bilateral (both sides) hip toggle procedure. This is open reduction and application of a synthetic ligament between the ball and socket. You can see the drilled tunnels (black lines) connecting the toggles (metal anchors).
Who performs the surgery?
As this is an act of veterinary surgery, only a veterinary surgeon can perform this. This is a technically demanding procedure and should only be performed by experienced orthopaedic surgeons. Our team of specialists have collectively been involved in 100’s of toggle surgery repairs over the years.
What is the recovery like?
Careful management after surgery is the key to success and it is vital that patients who undergo this surgery are managed diligently for the first 14 days after surgery to prevent damage to the operated hip. Exercise is progressively increases until off-lead exercise by approximately 6-8 weeks.
Patients will remain hospitalised for between 1-2 days post operatively depending on comfort, mobility and temperament. Once they are ready for home management, a dedicated rehabilitation and activity plan will be put in place.
Key elements of home management during the first 6 weeks include:
Room or cage confinement during unsupervised periods
Non slip flooring
Leash controlled walking activity only
What is the outcome after hip dislocation?
The success rate for hip dislocation surgery is >90%, and most patients are more comfortable within a few days to weeks of surgery. We expect most patients to return to full activity assuming there are no complications.
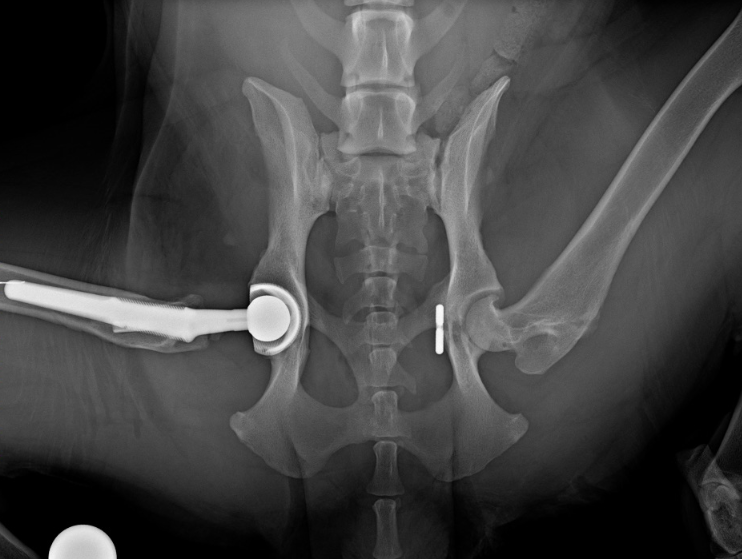
Rosie underwent a THR in 2018 and hip toggle in 2017 for atraumatic hip dislocation. She made a superb recovery.
What are the potential complications with hip dislocation
The major complications encountered with hip dislocation include:
repeat dislocation of the hip (rare after surgery )
implant loosening or infection
ongoing osteoarthritis (likely without surgery, possible with surgery when conformation is suboptimal)
Are there alternatives to surgery?
Hobble therapy can be successful in the manage of caudal-ventral luxations.
I would like to know more - whats the next step?
We recommend making an appointment with any of our specialist surgeons. If you are not local to Brisbane, we are happy to discuss eligible cases over the phone as a preliminary step. Having a copy of your pets medical history submitted to the hospital in advance of this phone call is recommended.